Guide to NHS Dental Implant Eligibility for Over 60s
This comprehensive guide outlines the NHS eligibility criteria for dental implants for individuals aged over 60. It details the clinical requirements, common medical conditions, referral procedures, and expected waiting times for treatment. The guide aims to empower seniors by providing them with insights into realistic NHS dental treatment options, helping them make informed decisions regarding their dental health and what to expect when seeking dental implant services. Understanding these factors is crucial for seniors considering dental implants and navigating the NHS system efficiently.
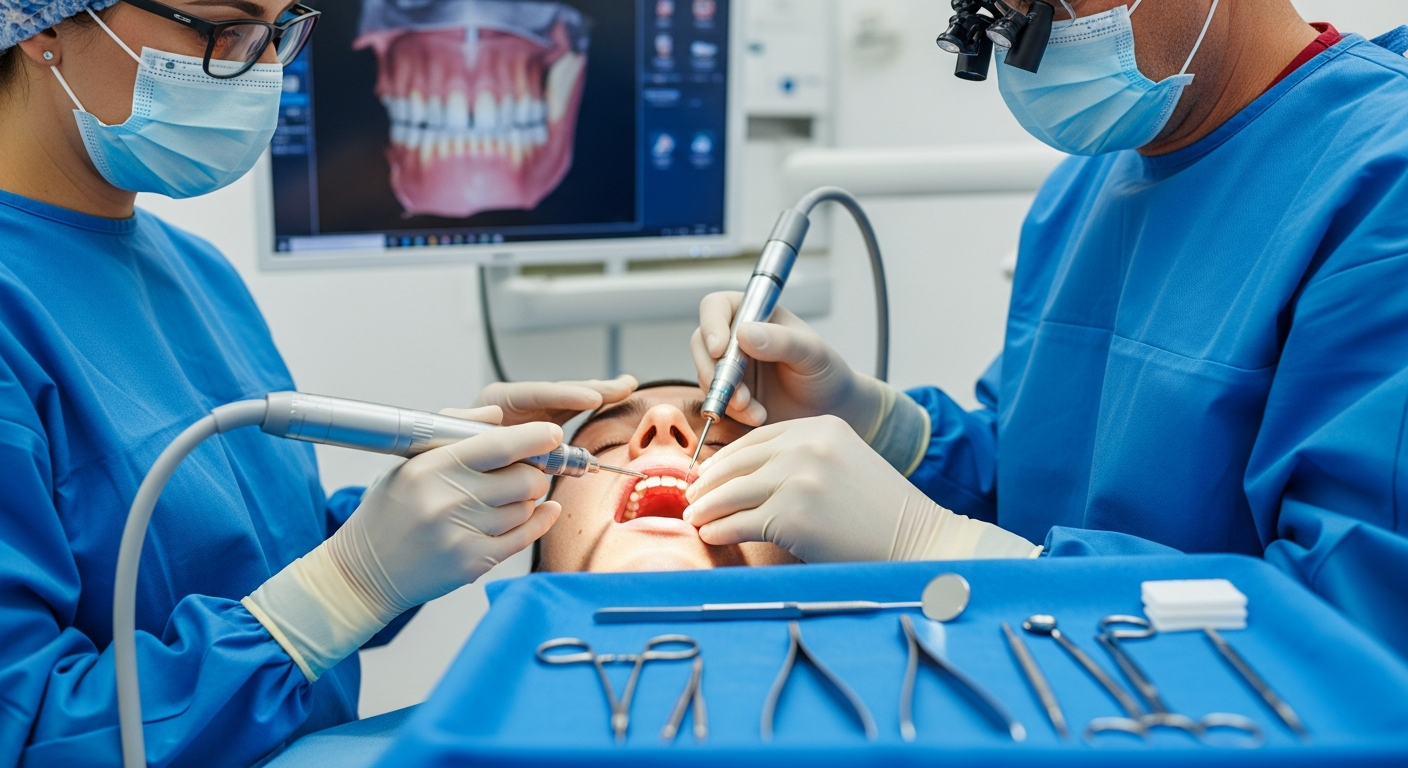
Dental implants represent a significant investment in oral health, offering a permanent solution for missing teeth. However, accessing this treatment through the NHS involves specific criteria and processes that many seniors may find challenging to understand. This comprehensive guide clarifies the pathway to obtaining dental implants for those over 60.
What are the NHS eligibility criteria for dental implants?
The NHS provides dental implants only in specific clinical circumstances, not for purely cosmetic reasons. Eligibility typically requires a clear clinical need, such as when you cannot wear dentures due to severe gagging reflex, when facial trauma has resulted in tooth loss, or when congenital conditions affect tooth development. Cancer treatment affecting the mouth or jaw may also qualify you for NHS-funded implants. Age alone does not determine eligibility; rather, your overall oral health, medical history, and the clinical necessity of the procedure are assessed. Most routine tooth replacements, even for seniors, fall outside NHS coverage and require private treatment. Your general health must be sufficient to undergo surgery, and you need adequate bone density to support implants. Smoking, uncontrolled diabetes, or certain medications may affect your suitability for the procedure.
What to expect during your dental consultation and assessment
Your journey begins with a comprehensive dental examination at an NHS practice. The dentist will evaluate your oral health, take X-rays or CT scans to assess bone structure, and review your medical history. This initial consultation determines whether you meet the clinical criteria for NHS funding. If you qualify, your dentist will refer you to a specialist oral surgeon or periodontist. During specialist assessment, expect detailed imaging, discussion of treatment options, and evaluation of any underlying health conditions that might affect surgery. The specialist will create a personalized treatment plan, explaining the procedure, timeline, and expected outcomes. This assessment phase can take several weeks to months, depending on the complexity of your case and the need for preparatory treatments like bone grafting. Be prepared to discuss your expectations, concerns, and any medications you take regularly.
Understanding NHS wait times and referral pathways
NHS dental implant procedures typically involve substantial waiting periods. After your initial assessment and approval, you may wait several months before treatment begins. Wait times vary significantly across different NHS trusts and regions, ranging from three to eighteen months or longer. The referral pathway starts with your general dentist, who submits a case to the local NHS commissioning body. If approved, you receive a referral to a hospital dental department or specialist clinic. Emergency cases or those with significant medical need may receive priority. During waiting periods, maintaining good oral hygiene and attending regular check-ups remains essential. Some patients require preparatory procedures like extractions or bone grafts before implant placement, which extends the overall timeline. Understanding that NHS resources are allocated based on clinical priority helps set realistic expectations about treatment schedules.
Financial options if implants aren’t covered by the NHS
When dental implants fall outside NHS coverage, several financial alternatives exist. Private dental treatment costs vary considerably depending on location, clinic reputation, and case complexity. Single implant procedures typically range from £1,500 to £3,000, while full-mouth restorations can exceed £20,000. Many private practices offer payment plans spreading costs over 12 to 60 months, making treatment more accessible. Dental insurance policies rarely cover implants for pre-existing conditions but may contribute if you’ve held coverage before tooth loss occurred. Some seniors explore dental tourism, traveling to countries with lower treatment costs, though this carries risks regarding follow-up care and quality assurance. Credit options specifically for medical procedures, such as healthcare credit cards, provide another route. Charitable organizations occasionally assist seniors with dental costs in cases of financial hardship.
| Provider Type | Typical Cost Range | Payment Options |
|---|---|---|
| NHS (if eligible) | Free to £282.80 (Band 3) | Upfront NHS charges |
| Private UK Clinic | £1,500 - £3,000 per implant | Payment plans, finance |
| Dental Schools | £800 - £1,500 per implant | Reduced fees, upfront |
| Overseas Clinics | £500 - £1,200 per implant | Typically upfront |
Prices, rates, or cost estimates mentioned in this article are based on the latest available information but may change over time. Independent research is advised before making financial decisions.
Preparing for dental implant surgery and recovery at home
Proper preparation significantly impacts surgical outcomes and recovery comfort. Before surgery, arrange transportation home as you cannot drive post-procedure. Stock your kitchen with soft foods like soups, yogurt, smoothies, and mashed vegetables for the first week. Purchase prescribed medications in advance, including antibiotics and pain relief. Prepare ice packs to reduce swelling and have clean gauze available for any bleeding. Clear your schedule for at least three days of rest following surgery. On surgery day, wear comfortable clothing and avoid wearing makeup or jewelry. Follow fasting instructions if receiving sedation. Post-surgery, expect swelling, minor bleeding, and discomfort for several days. Apply ice packs for 15-minute intervals during the first 48 hours. Maintain gentle oral hygiene, avoiding the surgical site initially. Eat soft foods and avoid hot liquids, alcohol, and smoking during healing. Most seniors return to normal activities within a week, though complete healing takes several months. Attend all follow-up appointments to monitor healing and address any complications promptly. Report excessive pain, prolonged bleeding, or signs of infection immediately.
Conclusion
Accessing dental implants through the NHS requires meeting specific clinical criteria, navigating referral pathways, and often accepting significant wait times. For those over 60, understanding these processes and exploring alternative financial options when NHS coverage isn’t available ensures informed decision-making about oral health. Whether pursuing NHS treatment or private care, thorough preparation and realistic expectations contribute to successful outcomes and improved quality of life through restored dental function.




